A key principle of advancing scientific discourse is the opportunity scientists have to comment on, challenge or seek clarification of research studies following their publication.
Some esteemed journals such as the The Lancet have guidelines that make immediate correction of all identified errors of fact “mandatory”.
Yet some years after the authors of two highly influential studies recommending significant reductions in red meat consumption acknowledged numerous errors after having their studies challenged through the post-publication process, no corrections have been applied to the published papers.
This is despite “considerable concern” about the quality and transparency of their input data, validity of their assumptions and appropriateness of statistic modelling used, according to a newly published paper by a leading academic.
As a consequence the reports continue to be extensively cited, and erroneously influence food policy decisions and international dietary guidelines, and support dietary advice that would not meet nutritional requirements for adults and risks causing malnutrition in children.
A new paper published in the npj Science of Food journal this week, authored by Dr Alice Stanton of the Royal College of Surgeons in Ireland, highlights multiple errors and limitations in two highly influential reports that recommend significant reductions in red meat consumption.
Among concerns with the Global Burden of Disease 2019 Risk Factors Study and the EAT-Lancet planetary health reference diet is that they do not recognise or address the lesser bioavailability of protein and key micronutrients from plant-source foods versus animal-source foods.
Dr Stanton’s article states that red and processed meats are rich in all essential amino acids and in many commonly lacking micronutrients, including iron, zinc, vitamin B12 and vitamin D3 19–21.
“Whilst red and processed meats are not the only sources for these nutrients, for many populations worldwide, they are the most important bioavailable sources.
“If the current public health message advising moderate consumption of red and processed meats, as part of a healthy balanced diet, was to be replaced by GBD 2019 guidance that any intake of such meats was harmful, it is highly likely that the prevalence of child and maternal malnutrition, iron deficiency anaemia, and elderly sarcopenia, would be greatly increased.”
She also singled out concerns with the GBD 2019 Risk Factors Study setting the theoretical minimum risk exposure level (TMREL) for red and processed meats to zero.
“This was very puzzling, as the contribution of moderate consumption of red and processed meats to nutrient adequacy, appeared to be totally ignored,” Dr Stanton writes.
Importantly, the collaborators who developed the GBD 2019 risk factor study had since responded to this issue, and had confirmed that the TMREL for unprocessed red meat in future reports will not be zero.
“Even more recently, they have stated that the 95% uncertainty interval for this estimate is very wide (0–200 g/day)11 – this indicates that the optimal intake of red meat could be as high as 200 g a day.”
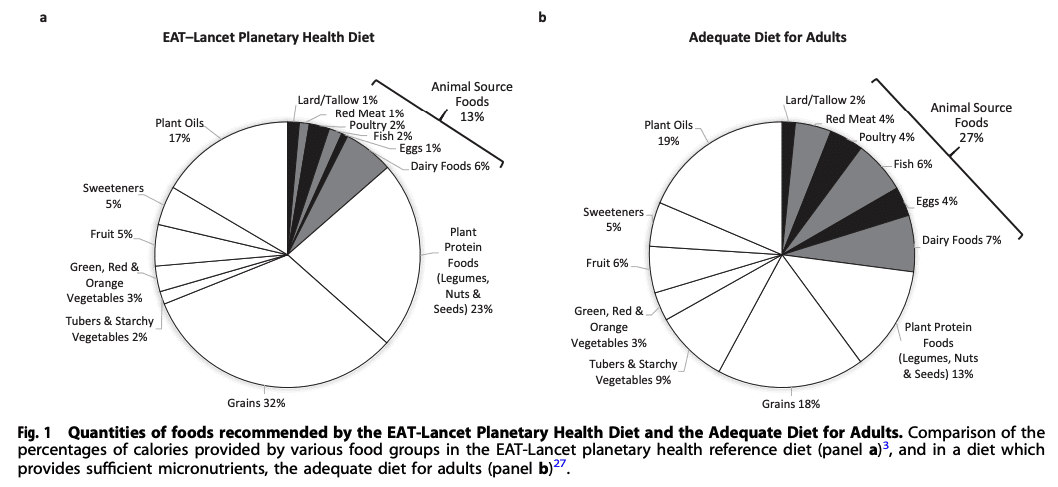
The EAT-Lancet planetary health reference diet published in 2019 allows low quantities of red or processed meats and eggs to be consumed, and includes moderate amounts of seafood and poultry.
However the diet largely consists of vegetables, fruits, whole grains, legumes, nuts and unsaturated plant oils, and only 13 percent of calories are from animal-source foods.
When questioned whether the considerable limitation of animal-source foods in the diet would negatively impact on protein and micronutrient adequacy, particularly for women, children and the elderly, and would result in adverse consequences for developing and aging brains, some of the EAT-Lancet Commissioners acknowledged that version of the diet would indeed result in significant essential micronutrient shortfalls, Dr Stanton said.
“It appears that insufficient attention was paid to the latest evidence on recommended nutrient intakes, and to the differences in micronutrient bioavailability from plant-source foods versus animal-source foods.
“In order to achieve micronutrient adequacy, intakes of animal-source foods would have to be doubled, accounting for at least 27 percent of calories, and intakes of phytates-rich plant-sourced foods, such as whole grains, pulses and nuts, would need to be considerably reduced.”
Compared with the GBD 2017 estimates, the GBD in 2019 increased the estimated disease burden attributed to diets high in unprocessed red meat by a factor of 36 times.
At the same time it lowered the disease burden attributed to diets low in fruit, nuts and seeds, vegetables, seafood omega-3 fatty acides, polyunsaturated fatty acids, vitamin A or zinc by more than 50 percent.
Why the considerable changes in just two years?
While all previous GBD analyses, including the GBD 2017 analysis, used data from systematic reviews and meta-analyses, Dr Stanton said the evidence for the 2019 dietary risk factor estimates came from “in house, newly conducted, systematic reviews and meta-regressions”.
These analyses had not been peer-reviewed nor published, and no assessments of certainty were documented.”
Dr Stanton, along with many other scientists, including representatives of the Academy of Nutrition Sciences and the World Cancer Research Fund (WCRF), questioned the reliability of the dramatically changed 2019 estimates, and requested that the newly conducted systematic reviews be peer reviewed and published.
When finally published three years later, the overall conclusions were that there was “no or only very weak evidence that unprocessed red meat is associated with any increased risk”.
It may be tempting to assume such a clear finding has resulted in corrections to the GBD report and assurances that future versions will not perpetuate the same errors.
However, despite limitations and errors being publicly acknowledged by the EAT-Lancet and GBD authors, no corrections have been applied to the published papers, and the same estimates remain unchanged on their websites.
GBD collaborators have also indicated they intend include “such weak, uncertain and statistically insignificant evidence in future GBD estimates of deaths. They recently commented that their preliminary estimates for GBD 2021 remain on the order of several hundred thousand deaths attributable to red meat consumption”, Dr Stanton writes.
“As a consequence these reports continue to be extensively cited, and many research groups continue to use the uncorrected estimates of risk and optimal intakes of the GBD 2019 Risk Factors Study and the EAT-Lancet planetary health diet, in their modelling studies.”
At the same time other influential reports acknowledge the errors: “Recent reports from the Food and Agriculture Organisation of the United Nations and the World Health Organisation have recognised and highlighted the weaknesses and errors in the two reports.”
In response to a question from London newspaper the Telegraph, a spokesman for the Lancet Group said: “The GBD 2019 Article, EAT-Lancet Commission on Food, Planet, Health and Lancet Countdown on health and climate change reports were each published following independent, external peer-review. “Scientific discussion and debate are an important part of the scientific process, and the Lancet journals welcome responses from readers and the wider scientific community to content published in the journals.”
Click here to read Dr Alice Stanton’s article in the npj Science of Food journal
RELATED ARTICLES
Livestock systems “too precious” to become victim of simplification, reductionism
Lancet study faces renewed calls to amend red meat intake study